Neonatal sepsis
- Apr 2
- 3 min read
INTRODUCTION
Neonatal sepsis is a life-threatening infection in newborns (0–28 days) caused by bacteria, viruses, or fungi. It is a major cause of neonatal morbidity and mortality, especially in developing countries.
DEFINITION
Neonatal sepsis is defined as
A systemic infection occurring in infants within the first 28 days of life, confirmed by clinical signs and/or positive blood culture.
TYPES
Early-Onset Sepsis (EOS)
Occurs within first 72 hours of life
Usually from maternal infection
Late-Onset Sepsis (LOS)
Occurs after 72 hours to 28 days
Usually from hospital or community exposure
CAUSES
Common Organisms
Bacteria
Group B Streptococcus (GBS)
E. coli
Klebsiella
Staphylococcus aureus
Viruses
Herpes simplex virus (HSV)
Fungi
Candida
RISK FACTORS
Maternal Factors
Prolonged rupture of membranes (>18 hours)
Maternal fever during labor
Urinary tract infection
Chorioamnionitis
Poor antenatal care
Neonatal Factors
Low birth weight (<2.5 kg)
Prematurity
Birth asphyxia
Meconium aspiration
Invasive procedures (IV lines, ventilation)
CLINICAL MANIFESTATIONS
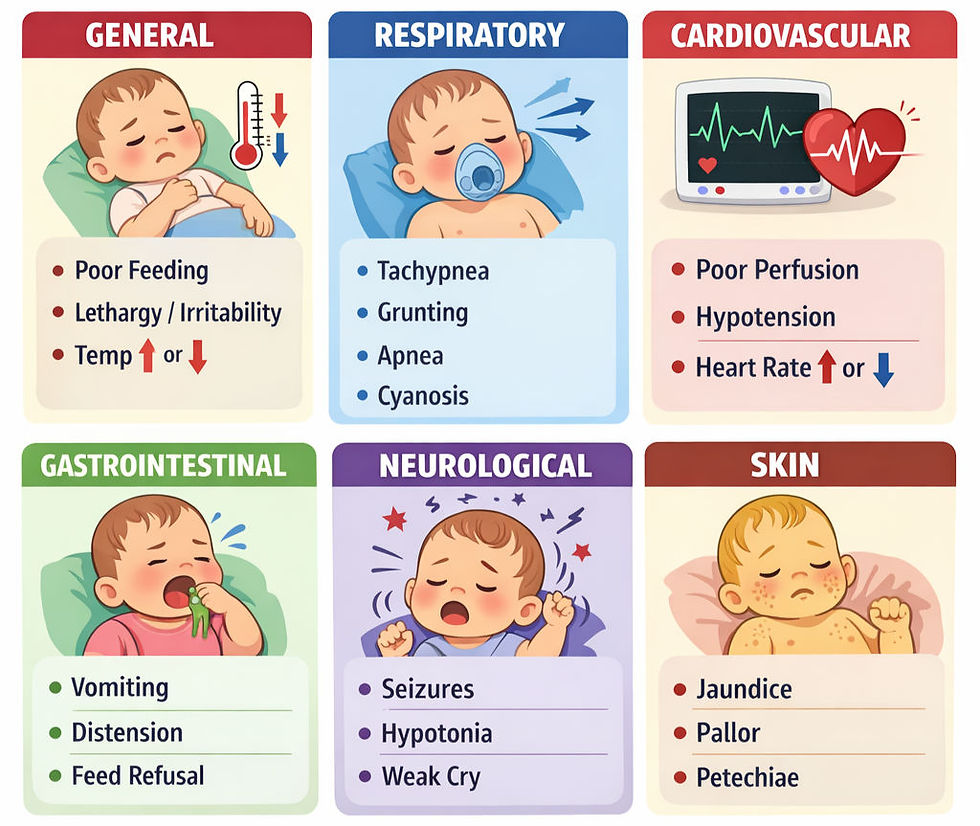
DIAGNOSIS
Laboratory Tests
Blood culture (gold standard)
Complete blood count (CBC)
↓ WBC or ↑ WBC
C-reactive protein (CRP)
Procalcitonin
Other Investigations
Lumbar puncture (for meningitis)
Chest X-ray (if respiratory symptoms)
Urine culture
Management
1. Supportive Care
Maintain temperature (warmth)
Oxygen therapy
IV fluids
Maintain blood glucose
Monitor vital signs
2. Antibiotic Therapy
(Start immediately—don’t wait for culture)
Empirical Treatment
Ampicillin + Gentamicin (most common)
If severe or resistant
Cefotaxime / Vancomycin (as per hospital protocol)
3. Specific Treatment
Antifungal (for Candida)
Antiviral (Acyclovir for HSV)
4. Nursing Management
Hand hygiene (infection control)
Monitor vital signs frequently
Maintain feeding (breastfeeding if possible)
Strict aseptic technique
Educate parents
COMPLICATIONS
Septic shock
Meningitis
Pneumonia
Disseminated intravascular coagulation (DIC)
Death
PREVENTION
Proper antenatal care
Clean delivery practices
Early breastfeeding
Infection control in NICU
Screening for maternal infections
🚀Here’s a short “exam trick” version for Neonatal Sepsis — super quick points you can remember :
🧸 Introduction
👉 Life-threatening infection in newborn (0–28 days)
📖 Definition
👉 Systemic infection with clinical signs ± positive blood culture.
🦠 Types
👉 Early-onset (≤72 hrs) – maternal origin
👉 Late-onset (>72 hrs) – hospital/community origin
⚡ Causes
👉 Bacteria (GBS, E. coli), virus (HSV), fungi (Candida)
⚠️ Risk Factors
👉 Maternal infection + PROM + prematurity + low birth weight
🧠 Clinical Manifestations
👉 Poor feeding, lethargy, temp instability, apnea, seizures
🔍 Diagnosis
👉 Blood culture (gold standard) + CBC + CRP
💊 Management
👉 Early antibiotics (Ampicillin + Gentamicin) + supportive care
👩⚕️ Nursing Care
👉 Maintain warmth, hygiene, monitor vitals, support feeding
🚨 Complications
👉 Shock, meningitis, DIC, death
🛡️ Prevention
👉 Clean delivery + antenatal care + infection control
🚀Here’s a set of 07 MCQs on Neonatal Sepsis for practice :
1. Neonatal sepsis is defined as:
A. Local infection in newborn
B. Systemic infection in newborn up to 28 days
C. Infection after 1 month
D. Only bacterial infection
✅ Answer: B
2. Early-onset neonatal sepsis occurs within:
A. 24 hours
B. 48 hours
C. 72 hours
D. 7 days
✅ Answer: C
3. Most common cause of early-onset neonatal sepsis:
A. Staphylococcus aureus
B. Group B Streptococcus
C. Candida
D. HSV
✅ Answer: B
4. Which is a major risk factor for neonatal sepsis?
A. High birth weight
B. Prolonged rupture of membranes
C. Normal delivery
D. Breastfeeding
✅ Answer: B
5. Gold standard investigation for neonatal sepsis:
A. CBC
B. CRP
C. Blood culture
D. X-ray
✅ Answer: C
6. First-line empirical treatment:
A. Paracetamol
B. Ampicillin + Gentamicin
C. Acyclovir
D. Antifungal
✅ Answer: B
7. Common clinical sign of neonatal sepsis:
A. Hyperactivity
B. Poor feeding
C. Weight gain
D. Increased sleep only
✅ Answer: B
Comments